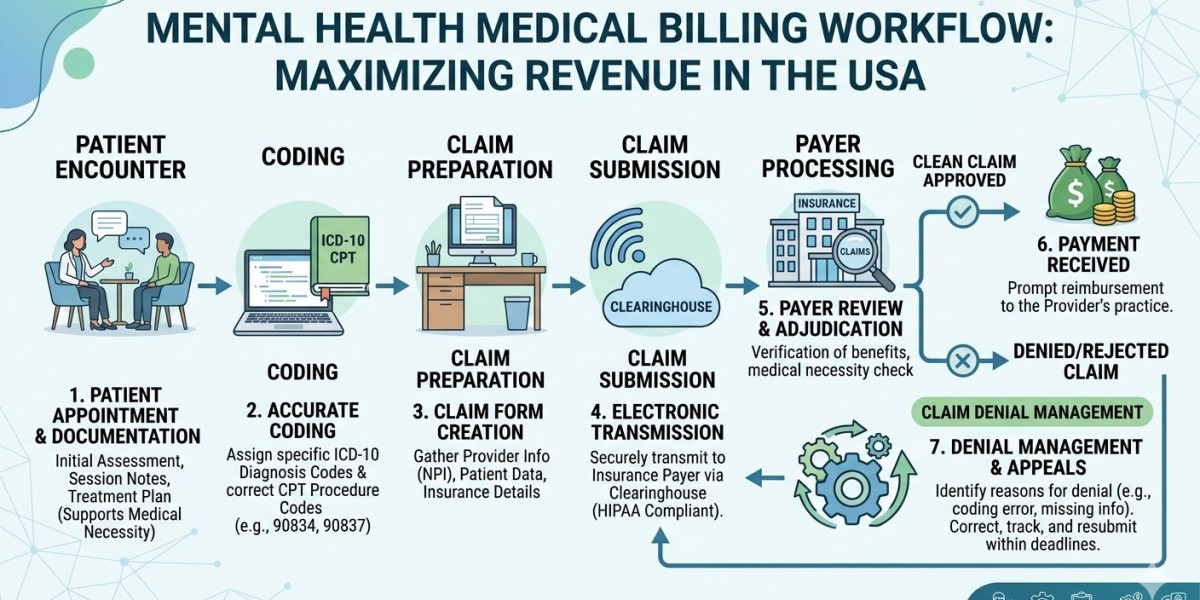
The demand for accurate and efficient mental healthcare administration is rising across the United States. As practices expand, managing billing, coding, and credentialing becomes more complex and time-consuming. This is where mental health billing and credentialing services play a critical role in ensuring smooth operations, faster reimbursements, and regulatory compliance.
Whether you are an independent therapist, a group practice, or a behavioral health clinic, understanding how these services work can significantly improve your revenue cycle and reduce administrative burden.
Introduction
Mental health professionals face unique challenges compared to other specialties. From therapy session documentation to insurance complexities, every step requires precision. Many providers struggle with claim denials, delayed payments, and credentialing issues that impact their financial stability.
To address these challenges, specialized mental health billing services and credentialing support have become essential. These services not only streamline administrative processes but also allow providers to focus on delivering quality patient care.
Why Mental Health Billing Is Different
Mental health billing is not the same as general medical billing. It involves specific codes, session-based billing, and strict payer guidelines.
- Therapy sessions are time-based, requiring accurate documentation
- Insurance policies vary widely for behavioral health coverage
- Frequent updates in compliance and coding rules
- High denial rates due to minor errors
Because of these factors, medical billing for mental health requires expertise and experience to ensure claims are processed correctly.
What Are Mental Health Billing and Credentialing Services
Mental health billing and credentialing services include a comprehensive set of administrative functions designed to manage the financial and compliance aspects of a practice.
These services typically cover:
- Insurance verification and eligibility checks
- Claim submission and tracking
- Payment posting and reconciliation
- Denial management and appeals
- Provider enrollment and credentialing
Credentialing ensures that providers are authorized to work with insurance companies, while billing ensures they get paid for their services.
Importance of Credentialing in Mental Health Practices
Credentialing is often overlooked but is a crucial component of practice growth. Without proper credentialing, providers cannot bill insurance companies.
Key benefits include:
- Access to a wider patient base through insurance networks
- Faster reimbursement cycles
- Compliance with payer requirements
- Increased trust and credibility
When combined with mental health medical billing, credentialing creates a strong foundation for financial success.
Key Components of Mental Health Billing Services
A reliable billing process involves multiple steps that must work seamlessly together.
Insurance Verification
Before any service is provided, verifying patient eligibility ensures that claims are not denied later.
Accurate Coding
Proper coding and billing for mental health services is essential. Errors in CPT or ICD codes can lead to claim rejection.
Claim Submission
Timely and clean claim submission reduces delays and improves cash flow.
Denial Management
Handling denied claims effectively is crucial to recovering lost revenue.
Payment Posting
Tracking payments accurately ensures transparency and proper financial reporting.
Billing for Mental Health Therapists
Therapists often face challenges in managing billing while maintaining their clinical workload. Billing for mental health therapists requires attention to session duration, therapy type, and payer guidelines.
Common challenges include:
- Managing multiple insurance providers
- Understanding therapy-specific billing codes
- Keeping up with regulatory changes
Outsourcing these tasks allows therapists to focus entirely on patient care while maintaining financial stability.
Benefits of Outsourced Billing for Mental Health
Many practices are now choosing outsourced billing for mental health to improve efficiency and reduce operational stress.
Here’s why outsourcing works:
- Reduces administrative workload
- Improves claim accuracy and acceptance rates
- Ensures compliance with regulations
- Provides access to billing experts
- Saves time and operational costs
Choosing the best outsource mental health billing and coding services can significantly enhance revenue performance.
How to Choose the Right Billing Partner
Selecting the right partner for billing services for mental health clinics is critical. Not all billing companies understand the nuances of behavioral health.
Consider the following factors:
- Experience in behavioral and mental health billing services
- Knowledge of insurance policies and compliance
- Transparent pricing models
- Strong reporting and analytics
- Proven track record of reducing denials
Some providers also look for a cheap outsource mental health billing company, but cost should never compromise quality and accuracy.
Medicare and Mental Health Billing
Billing Medicare requires strict adherence to guidelines. Billing Medicare for mental health services involves:
- Understanding covered services
- Using correct CPT and ICD codes
- Ensuring documentation meets Medicare standards
- Following timely filing requirements
Mistakes in Medicare billing can lead to audits and penalties, making expertise essential in this area.
Common Challenges in Mental Health Billing
Despite advancements, many practices still face challenges such as:
- High claim rejection rates
- Complex insurance requirements
- Delayed reimbursements
- Lack of trained staff
- Inefficient billing systems
These issues highlight the importance of professional billing services for mental health that can handle complexities efficiently.
How Mental Health Billing Services Improve Revenue Cycle
An optimized revenue cycle ensures consistent cash flow and financial stability.
Benefits include:
- Faster claim processing
- Reduced denials and rejections
- Improved patient billing experience
- Better financial reporting
- Increased profitability
Effective mental health billing transforms administrative challenges into growth opportunities.
Technology and Automation in Mental Health Billing
Modern billing solutions integrate technology to improve accuracy and efficiency.
Key advancements include:
- Electronic health records integration
- Automated claim submission
- Real-time eligibility verification
- Data analytics for performance tracking
These tools enhance the overall effectiveness of billing mental health services.
Why Specialized Billing Matters for Behavioral Health
General billing companies may not fully understand the unique requirements of mental health practices. Specialized providers offering behavioral and mental health billing services bring expertise that ensures compliance and efficiency.
They understand:
- Therapy-specific billing structures
- Insurance nuances for behavioral health
- Documentation requirements
- Compliance standards
This specialization leads to better financial outcomes and reduced stress for providers.
Conclusion
Managing billing and credentialing in mental health practices is both critical and complex. From insurance verification to claim submission and compliance, every step requires precision and expertise.
By leveraging professional mental health billing and credentialing services, providers can streamline operations, improve revenue, and focus on delivering quality care.
For practices looking to scale efficiently, partnering with a trusted provider like 247 Medical Billing Services can make a significant difference. With expertise in medical billing services, medical coding services, medical billing and coding services, revenue cycle management services, and credentialing services, they help mental health professionals achieve financial stability while maintaining compliance.
FAQs
What are mental health billing and credentialing services?
These services manage insurance billing, coding, and provider enrollment to ensure accurate reimbursements and compliance.
Why is credentialing important for mental health providers?
Credentialing allows providers to work with insurance companies and receive payments for their services.
Can I manage mental health billing on my own?
While possible, it is complex and time-consuming. Many providers prefer outsourcing for accuracy and efficiency.
What is included in mental health billing services?
Services include insurance verification, coding, claim submission, denial management, and payment posting.
How does outsourcing improve billing performance?
Outsourcing reduces errors, speeds up claim processing, and improves overall revenue cycle management.
Is Medicare billing different for mental health services?
Yes, it requires strict adherence to guidelines, proper documentation, and correct coding practices.